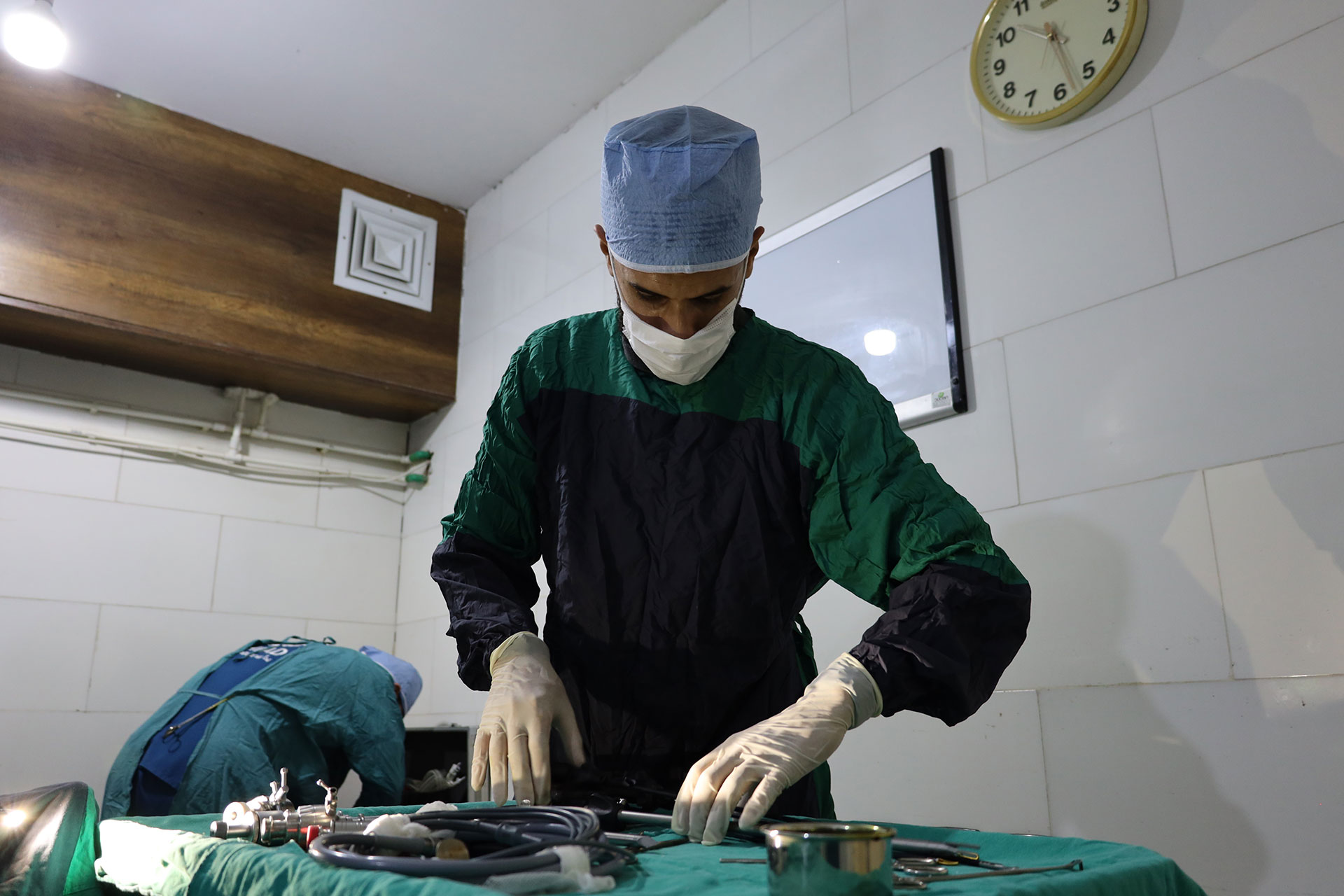
Reducing greenhouse gas emissions in a bariatric surgical unit is a complex but feasible project

Obesity, obesity surgery, and environment
Obesity per se is a major contributor to GHGe, in relation with the carbon footprint of food production and associated supply chain. The genesis of obesity thus significantly impacts GHGe worldwide. Regarding metabolic food waste (MFW), which is defined as the amount of food leading to excess body fat, Europe and North America were found to display the highest values for all three MFW footprints (i.e. carbon, water, and land footprints), being 14 times larger than in South Asia and South-East Asia12. The modern food environment, i.e. food availability, also strongly contributes to this genesis in any country13.
One would assume that a more or less significant part of this waste may be compensated to a large extent by weight loss, notably achieved by bariatric procedures. While there is no substantial evidence for this, a large body of arguments point to reduced medical costs after surgical weight loss, with therefore a favorable impact on the environment14.
Although bariatric procedures marginally contribute to lower resource consumption once patients have achieved sustained weight loss, an argument can be put forward in favor of such interventions, therefore justifying coverage by health insurances: the markedly increased well-being of the obese population15. In other words, fighting the stigma that is often associated with obesity is beneficial to this population, since this stigma prevents obese patients from gaining easy access to treatments such as bariatric surgery16.
Two current trends may adversely affect this reasoning: (1) the relatively aggressive approach towards Stage I obesity [body mass index (BMI) 30–35], with obesity surgery claiming success in those patients when affected by a comorbidity, typically type 2 diabetes17, hence the assertion that metabolic surgery should be strongly promoted and offsets the costs of treating such conditions; (2) the relative extension of robotic surgery in this field also significantly impacts GHGe, as previously shown in gynecological surgery10 or other types of surgery11.
Looking for opportunities and compromises
Other strategies pursuing common goals are currently being considered. On the one hand, “green surgical innovation”18 suggests that evaluating new surgical devices or new surgical options in general, such as robotics10,11 or digitalized options, could benefit from the strict analysis of their carbon footprint, which thus determines whether a new strategy/device should be implemented or not. This is questionable, since innovations and environment may remain compatible. On the other hand, others rightly point out that surgical issues have boundaries that go beyond the strict perimeter of the OR19, or even suggest a much broader move that encompasses several items in order to build sustainable and resilient surgical systems, possibly at the level of a geographical area, e.g. the West Pacific region, including infrastructure, service delivery, finance, information systems, health workforce, and governance20. One may object that health systems are closely interconnected throughout the world, for example when it comes to the workforce, and that such definitions may be vague enough to hamper real and coordinated efforts.
As noted by Rizan et al.3, the numbers are difficult to interpret because the various studies have different frameworks and use different references, with the authors placing emphasis on the various choices that can be debated, e.g. whether or not including anesthesiology, energy mix, life cycle analysis, etc. Hence, we suggest acting upon what is currently within reach at a given time and evaluating the progress that can be achieved at various levels. We propose to start from a given situation in a hospital and try to improve different scores, thereby contributing to a more global effort including recycling, re-processing, eliminating single-use items whenever possible, energy saving, and minimizing instrument use and anesthetic gas. It is common to feel that others should make environmental efforts before we do, or in other words, that other fields have a more detrimental impact on the environment than our own. In view of the substantial contribution of the Scope 2 (energy) to GHGe as compared to the others, one may claim to be powerless or favor green-washing options and focus on good intentions rather than real actions. Likewise, many choose to blend environmental issues with social issues when presenting results, which is politically relevant (at least regarding the so-called “social and environmental responsibility”), but probably scientifically irrelevant in the medical field.
Yet, it is interesting to look at other fields whose environmental strategy is nowadays being questioned, such as the automobile industry, fashion industry, construction, computer software and internet, etc. How fast are efforts being made and should we follow the same path? What kind of pressure is applied in each case? These are difficult questions, and it may be best that everyone acts on their own behalf, regardless of what others do.
For now, we overlooked the final aspect of GHGe in patients at the very end of the surgical process, i.e. considering the economical long-term benefits of weight loss, which offset the initial costs in many studies. For instance, the decrease in drug costs has been evaluated: In a meta-analysis performed by Lopes et al. in 2015, the mean reduction in total drug costs was estimated at 49.8% over a follow-up duration of 6–72 months after bariatric surgery21. Yet, such studies are lacking for GHGe, and we need benchmarks. One study has been conducted in the field of esophageal reflux surgery, showing that the cost–benefit ratio was not favorable up to 9 years after surgery22. Further studies are warranted to assess the benefits of GHGe reduction in the bariatric field.
Lastly, we addressed what could be called the “obesity debt”, i.e. the food waste associated with overweight and obesity, which amounts to 140 M tons/year according to Totti et al.12. This does not impede the efforts towards weight loss, on the contrary, but it could be an incentive to favor less energy-consuming methods, e.g. endoscopic solutions rather than typical laparoscopic surgical options23. While an ultimatum like the EU ban of combustion-engine cars by 2035 is barely conceivable, it makes sense to promote incentives to develop less impacting technologies such as endoscopic bariatric methods, perhaps associated with new drugs (GLP-1 receptor agonists).
There is no reason why bariatric surgery would be more or less environmentally friendly according to BMI range; yet adding more patients to the surgical workflow seems unfriendly to the same environment, particularly if alternative and sound options exist for those patients (drugs, endoscopy, etc.), which is the case for lower BMI patients, and even for selected higher BMI patients and/or unwilling to undergo surgery. To put it differently: such treatments, that are explicitly non-surgical, entail less GHGe, and are therefore more likely to concern this range of BMI (30–35). However, when surgery is performed in these patients, it does not mean more GHGe, but those could have been spared if surgery had not been the primary option.
link