Effect of systematic nursing on scar appearance following radical thyroidectomy: a retrospective cohort analysis
Surgery is the most effective treatment for thyroid cancer, which is prevalent in China2,3. However, surgery always leaves a long, linear, disfiguring scar. Patients with thyroid cancer have relatively good prognoses after surgical resection. Many studies have focused on new approaches to combat scar formation with the reduction in patient concerns about thyroid tumors in recent years5. Most of these studies used either single or combination therapies6. Although these approaches have achieved certain effects within a certain period, the compliance rate of these patients may not be high, especially regarding invasive treatments or nursing measures. Patient education on scarring should be regular and detailed. However, comprehensive nursing guidance for postoperative scar management are not usually available for patients with thyroid cancer. To help patients understand every key step in antiscar nursing better, our nursing team developed the first systematic and comprehensive nursing guide and evaluated its effectiveness.
Incisions for thyroid cancer are mostly made along the skin lines of the neck. Hence, post-operative neck scarring is generally considered acceptable. Incision healing is divided into inflammation, proliferation, and remodeling processes. The remodeling stage is the most important stage that determines the quality of scar formation, which starts three weeks after incision formation and lasts 6 months4. Kathy et al.7 found that patients were concerned about scarring within a year of thyroid cancer surgery. Therefore, long-term observation and management are required to achieve satisfactory post-operative scars. Postoperative incision nursing care should be continued for a year8.
In our study, the enrolled female patients were followed up for 12 months, and the scarring quality of the patients was evaluated in detail and quantified using the VSS. Systematic nursing guidance were established according to the time after surgery (1st month; 2nd − 6th months; 7th − 12th months). All measures in the systematic nursing guides were noninvasive, which enhanced patient compliance. Since the follow-up lasted for a year, our nurses reminded the patients of the key nursing points monthly to increase their compliance, which was part of the systematic nursing guide. As part of the systematic nursing guidance, monthly reminders were provided to patients to reinforce key aspects of postoperative care. The guidance focused on three main components: Life customs: Patients were advised to avoid activities that might cause excessive tension or friction on the incision site, such as vigorous neck movements or sleeping without proper neck support. Maintaining good rest and avoiding stress were also encouraged, as psychological well-being can influence wound healing. Eating habits: A balanced diet rich in protein, vitamins (especially A and C), and trace elements like zinc was emphasized to promote skin regeneration and reduce the risk of abnormal scarring. Spicy and allergenic foods were discouraged, as they may contribute to local inflammation or delayed healing. Tension-reducing devices: The use of silicone gel sheets and medical tape was encouraged early in recovery to minimize mechanical stress on the incision and prevent hypertrophic scarring. These combined measures aimed to improve compliance, support wound healing, and reduce the incidence of hypertrophic scars or keloids9,10,11,12.
In previous studies, tension control and silicone gel were the most common methods for preventing scar formation due to their convenience and simplicity13,14,15,16. Patients in the experimental group reported no adverse impact on their lives or quality of life from using tension-reducing tape and silicone gel. However, they were willing to follow our guidance because they felt well taken care of by the monthly reminders from the nurses. By the 12th month after surgery, the patients in the experimental group were more satisfied with their scarring appearance and nursing care.
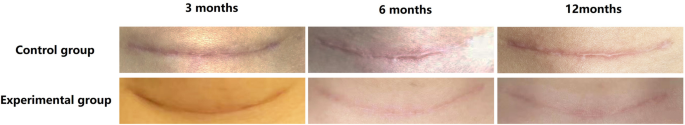
Previous studies have indicated many factors that could contribute to scar formation and appearance, including inflammation17,18, tension19, suture skills20, allergic diseases21, and individual lifestyle habits22. Several recent studies have focused on new approaches to combat scar formation, most of which use single or combination therapies. The VSS is currently the most frequently used scar assessment scale13,14 and is linked with quality of life1. Six aspects were used to evaluate scar conditions: pigmentation, vascularization, thickness, pliability, pain, and itching. Pigmentation is related to ultraviolet rays; therefore, sunscreen is the most effective way to lower the pigmentation score, as shown in our 6th and 12th postoperative month results. Vascularization is key in assessing scar formation and development23,24. Compared with the control group, the vascularization scores at the 6th and 12th post-operative months were much lower in the experimental group; however, no significant difference was found in the 3rd postoperative month. This indicates that improvement in scar vascularization by comprehensive nursing takes at least six months. Thickness and pliability represent scar maturation25. The scores for thickness and pliability in the experimental group were lower than those in the control group, indicating that comprehensive nursing improved scar maturation in the early stages of post-operative scar formation. Symptoms such as pain and itching usually affect patients’ quality of life after surgery26. Patients in the experimental group had no obvious complaints of pain or itching in the 6th month, indicating that a comprehensive nursing strategy can improve patient recovery and quality of life.
According to our results, systematic nursing guides have a promising effect on reducing scar formation and increasing patient satisfaction and are comprehensive, understandable, and practical. However, spontaneous discontinuation of systematic nursing guides may lead to the failure of anti-scar therapy. To solve this problem and increase patient compliance, we reminded patients monthly of the anti-scar key points. Although this might have increased the nurses’ workload, satisfactory results were achieved.
It is important to acknowledge the limitations of this study. First, the sample size was limited, which may impact the generalizability of the findings to a larger and more diverse population. Additionally, the study does not provide information about the long-term effects or whether the benefits persist over a more extended period. Despite using monthly reminders to enhance patient compliance, there were challenges in ensuring that all patients followed the systematic nursing guidance consistently. Although this study shows promise, its limitations need to be acknowledged when interpreting the findings.
link