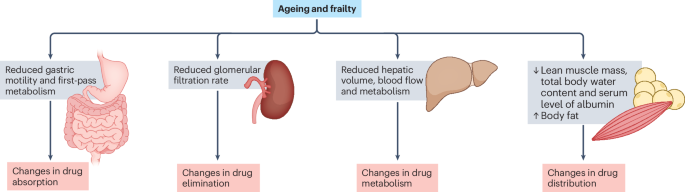
Optimizing cardiovascular pharmacotherapy in older adults with frailty
Heuberger, R. A. The frailty syndrome: a comprehensive review. J. Nutr. Gerontol. Geriatrics 30, 315–368 (2011).
Google Scholar
Clegg, A., Young, J., Iliffe, S., Rikkert, M. O. & Rockwood, K. Frailty in elderly people. Lancet 381, 752–762 (2013).
Google Scholar
Rockwood, K., Mitnitski, A., Song, X., Steen, B. & Skoog, I. Long-term risks of death and institutionalization of elderly people in relation to deficit accumulation at age 70. J. Am. Geriatrics Soc. 54, 975–979 (2006).
Google Scholar
Fried, L. P. et al. Frailty in older adults: evidence for a phenotype. J. Gerontol. A Biol. Sci. Med. Sci. 56, M146–M156 (2001).
Google Scholar
Kim, D. H. & Rockwood, K. Frailty in older adults. N. Engl. J. Med. 391, 538–548 (2024).
Google Scholar
Lang, P. O., Michel, J. P. & Zekry, D. Frailty syndrome: a transitional state in a dynamic process. Gerontology 55, 539–549 (2009).
Google Scholar
Searle, S. D., Mitnitski, A., Gahbauer, E. A., Gill, T. M. & Rockwood, K. A standard procedure for creating a frailty index. BMC Geriatr. 8, 24 (2008).
Google Scholar
Rockwood, K. & Mitnitski, A. Frailty defined by deficit accumulation and geriatric medicine defined by frailty. Clin. Geriatric Med. 27, 17–26 (2011).
Google Scholar
Ijaz, N. et al. Interventions for frailty among older adults with cardiovascular disease: JACC state-of-the-art review. J. Am. Coll. Cardiol. 79, 482–503 (2022).
Google Scholar
James, K. et al. Frailty and cardiovascular health. J. Am. Heart Assoc. 13, e031736 (2024).
Google Scholar
O’Caoimh, R. et al. Prevalence of frailty in 62 countries across the world: a systematic review and meta-analysis of population-level studies. Age Ageing 50, 96–104 (2021).
Google Scholar
O’Caoimh, R. et al. Prevalence of frailty at population level in European ADVANTAGE Joint Action Member States: a systematic review and meta-analysis. Ann. Ist. Super. Sanita 54, 226–238 (2018).
Google Scholar
Perera, V., Bajorek, B. V., Matthews, S. & Hilmer, S. N. The impact of frailty on the utilisation of antithrombotic therapy in older patients with atrial fibrillation. Age Ageing 38, 156–162 (2009).
Google Scholar
Richter, D. et al. Frailty in cardiology: definition, assessment and clinical implications for general cardiology. A consensus document of the Council for Cardiology Practice (CCP), Association for Acute Cardio Vascular Care (ACVC), Association of Cardiovascular Nursing and Allied Professions (ACNAP), European Association of Preventive Cardiology (EAPC), European Heart Rhythm Association (EHRA), Council on Valvular Heart Diseases (VHD), Council on Hypertension (CHT), Council of Cardio-Oncology (CCO), Working Group (WG) Aorta and Peripheral Vascular Diseases, WG e-Cardiology, WG Thrombosis, of the European Society of Cardiology, European Primary Care Cardiology Society (EPCCS). Eur. J. Prev. Cardiol. 29, 216–227 (2022).
Google Scholar
Veronese, N. et al. Risk of cardiovascular disease morbidity and mortality in frail and pre-frail older adults: results from a meta-analysis and exploratory meta-regression analysis. Ageing Res. Rev. 35, 63–73 (2017).
Google Scholar
Cappola, A. R., Xue, Q. L. & Fried, L. P. Multiple hormonal deficiencies in anabolic hormones are found in frail older women: the Women’s Health and Aging studies. J. Gerontol. A Biol. Sci. Med. Sci. 64, 243–248 (2009).
Google Scholar
Hyde, Z. et al. Low free testosterone predicts frailty in older men: the health in men study. J. Clin. Endocrinol. Metab. 95, 3165–3172 (2010).
Google Scholar
Mulero, J., Zafrilla, P. & Martinez-Cacha, A. Oxidative stress, frailty and cognitive decline. J. Nutr. Health Aging 15, 756–760 (2011).
Google Scholar
Newman, A. B. et al. Associations of subclinical cardiovascular disease with frailty. J. Gerontol. A Biol. Sci. Med. Sci. 56, M158–M166 (2001).
Google Scholar
Damluji, A. A. et al. Frailty and cardiovascular outcomes in the National Health and Aging Trends Study. Eur. Heart J. 42, 3856–3865 (2021).
Google Scholar
Shrauner, W. et al. Frailty and cardiovascular mortality in more than 3 million US Veterans. Eur. Heart J. 43, 818–826 (2021).
Google Scholar
Ekerstad, N. et al. Frailty is independently associated with short-term outcomes for elderly patients with non-ST-segment elevation myocardial infarction. Circulation 124, 2397–2404 (2011).
Google Scholar
Bo, M. et al. Health status, geriatric syndromes and prescription of oral anticoagulant therapy in elderly medical in-patients with atrial fibrillation: a prospective observational study. Int. J. Cardiol. 187, 123–125 (2015).
Google Scholar
Lee, D. H., Buth, K. J., Martin, B. J., Yip, A. M. & Hirsch, G. M. Frail patients are at increased risk for mortality and prolonged institutional care after cardiac surgery. Circulation 121, 973–978 (2010).
Google Scholar
Singh, M. et al. Influence of frailty and health status on outcomes in patients with coronary disease undergoing percutaneous revascularization. Circ. Cardiovasc. Qual. Outcomes 4, 496–502 (2011).
Google Scholar
Ambler, G. K. et al. Effect of frailty on short- and mid-term outcomes in vascular surgical patients. Br. J. Surg. 102, 638–645 (2015).
Google Scholar
Singh, I. et al. Predictors of adverse outcomes on an acute geriatric rehabilitation ward. Age Ageing 41, 242–246 (2012).
Google Scholar
Cacciatore, F. et al. Long-term mortality in frail elderly subjects with osteoarthritis. Rheumatology 53, 293–299 (2014).
Google Scholar
Le Maguet, P. et al. Prevalence and impact of frailty on mortality in elderly ICU patients: a prospective, multicenter, observational study. Intensive Care Med. 40, 674–682 (2014).
Google Scholar
Conroy, S. & Dowsing, T. The ability of frailty to predict outcomes in older people attending an acute medical unit. Acute Med. 12, 74–76 (2013).
Google Scholar
Cacciatore, F. et al. Frailty predicts long-term mortality in elderly subjects with chronic heart failure. Eur. J. Clin. Investig. 35, 723–730 (2005).
Google Scholar
Hubbard, R. E., O’Mahony, M. S. & Woodhouse, K. W. Medication prescribing in frail older people. Eur. J. Clin. Pharmacol. 69, 319–326 (2013).
Google Scholar
Yao, A., Gao, L., Zhang, J., Cheng, J. M. & Kim, D. H. Frailty as an effect modifier in randomized controlled trials: a systematic review. J. Gen. Intern. Med. 39, 1452–1473 (2024).
Google Scholar
Zheng, Y. et al. Effect of oral anticoagulants in atrial fibrillation patients with polypharmacy: a meta-analysis. Thromb. Haemost. 125, 166–177 (2025).
Google Scholar
Romiti, G. F. et al. Clinical complexity domains, anticoagulation, and outcomes in patients with atrial fibrillation: a report from the GLORIA-AF Registry Phase II and III. Thromb. Haemost. 122, 2030–2041 (2022).
Google Scholar
Grymonprez, M., Petrovic, M., De Backer, T. L., Steurbaut, S. & Lahousse, L. The impact of polypharmacy on the effectiveness and safety of non-vitamin K antagonist oral anticoagulants in patients with atrial fibrillation. Thromb. Haemost. 124, 135–148 (2024).
Google Scholar
Raphael, D. et al. Frailty: a public health perspective. Can. J. Public. Health 86, 224–227 (1995).
Google Scholar
Kanapuru, B. & Ershler, W. B. Inflammation, coagulation, and the pathway to frailty. Am. J. Med. 122, 605–613 (2009).
Google Scholar
Savelieva, I. et al. EHRA expert consensus document on the management of arrhythmias in frailty syndrome, endorsed by the Heart Rhythm Society (HRS), Asia Pacific Heart Rhythm Society (APHRS), Latin America Heart Rhythm Society (LAHRS), and Cardiac Arrhythmia Society of Southern Africa (CASSA). Europace 25, 1249–1276 (2023).
Google Scholar
Walker, D. M. et al. Editor’s choice — Frailty and the management of patients with acute cardiovascular disease: a position paper from the acute cardiovascular care association. Eur. Heart J. Acute Cardiovasc. Care 7, 176–193 (2018).
Google Scholar
Visseren, F. L. J. et al. 2021 ESC Guidelines on cardiovascular disease prevention in clinical practice: developed by the Task Force for Cardiovascular Disease Prevention in Clinical Practice with representatives of the European society of Cardiology and 12 medical societies with the special contribution of the European Association of Preventive Cardiology (EAPC). Eur. Heart J. 42, 3227–3337 (2021).
Google Scholar
McEvoy, J. W. et al. 2024 ESC guidelines for the management of elevated blood pressure and hypertension: developed by the Task Force on the Management of Elevated Blood Pressure and Hypertension of the European Society of Cardiology (ESC) and endorsed by the European Society of Endocrinology (ESE) and the European Stroke Organisation (ESO). Eur. Heart J. 45, 3912–4018 (2024).
Google Scholar
Grundy, S. M. et al. 2018 AHA/ACC/AACVPR/AAPA/ABC/ACPM/ADA/AGS/APhA/ASPC/NLA/PCNA guideline on the management of blood cholesterol: a report of the American College of Cardiology/American Heart Association Task Force on Clinical Practice Guidelines. Circulation 139, e1082–e1143 (2019).
Google Scholar
Hilmer, S. N., Wu, H. & Zhang, M. Biology of frailty: implications for clinical pharmacology and drug therapy in frail older people. Mech. Ageing Dev. 181, 22–28 (2019).
Google Scholar
Wynne, H. A. et al. The association of age and frailty with the pharmacokinetics and pharmacodynamics of metoclopramide. Age Ageing 22, 354–359 (1993).
Google Scholar
Hilmer, S. N. & Kirkpatrick, C. M. J. New horizons in the impact of frailty on pharmacokinetics: latest developments. Age Ageing 50, 1054–1063 (2021).
Google Scholar
Zazzara, M. B., Palmer, K., Vetrano, D. L., Carfì, A. & Onder, G. Adverse drug reactions in older adults: a narrative review of the literature. Eur. Geriatr. Med. 12, 463–473 (2021).
Google Scholar
O’Brien, T. D., Roberts, J., Brackenridge, G. R. & Lloyd, W. H. Some aspects of community care of the frail and elderly: the need for assessment. Gerontol. Clin. 10, 215–227 (1968).
Google Scholar
Winograd, C. H., Gerety, M. B., Brown, E. & Kolodny, V. Targeting the hospitalized elderly for geriatric consultation. J. Am. Geriatrics Soc. 36, 1113–1119 (1988).
Google Scholar
Deng, Y. & Sato, N. Global frailty screening tools: review and application of frailty screening tools from 2001 to 2023. Intractable Rare Dis. Res. 13, 1–11 (2024).
Google Scholar
Azzopardi, R. V. et al. Linking frailty instruments to the international classification of functioning, disability, and health: a systematic review. J. Am. Med. Dir. Assoc. 17, 1066.e1–1066.e11 (2016).
Google Scholar
Ma, L. Current situation of frailty screening tools for older adults. J. Nutr. Health Aging 23, 111–118 (2019).
Google Scholar
de Vries, N. M. et al. Outcome instruments to measure frailty: a systematic review. Ageing Res. Rev. 10, 104–114 (2011).
Google Scholar
Martin, F. C. & Brighton, P. Frailty: different tools for different purposes? Age Ageing 37, 129–131 (2008).
Google Scholar
Dent, E. et al. The Asia-Pacific clinical practice guidelines for the management of frailty. J. Am. Med. Dir. Assoc. 18, 564–575 (2017).
Google Scholar
NCD Risk Factor Collaboration (NCD-RisC) Worldwide trends in hypertension prevalence and progress in treatment and control from 1990 to 2019: a pooled analysis of 1201 population-representative studies with 104 million participants. Lancet 398, 957–980 (2022).
Vetrano, D. L. et al. Hypertension and frailty: a systematic review and meta-analysis. BMJ Open. 8, e024406 (2018).
Google Scholar
Williamson, J. D. et al. Intensive vs standard blood pressure control and cardiovascular disease outcomes in adults aged ≥75 years: a randomized clinical trial. JAMA 315, 2673–2682 (2016).
Google Scholar
National Institute for Health and Care and Excellence. Hypertension in Adults: Diagnosis and Management. NICE Guideline NG136. (NICE, 2023).
Qaseem, A. et al. Pharmacologic treatment of hypertension in adults aged 60 years or older to higher versus lower blood pressure targets: a clinical practice guideline from the American College of Physicians and the American Academy of Family Physicians. Ann. Intern. Med. 166, 430–437 (2017).
Google Scholar
Gabb, G. M. et al. Guideline for the diagnosis and management of hypertension in adults — 2016. Med. J. Aust 205, 85–89 (2016).
Google Scholar
Goupil, R. et al. Hypertension Canada guideline for the diagnosis and treatment of hypertension in adults in primary care. CMAJ 197, E549–E564 (2025).
Google Scholar
Jones, D. W. et al. 2025 AHA/ACC/AANP/AAPA/ABC/ACCP/ACPM/AGS/AMA/ASPC/NMA/PCNA/SGIM Guideline for the Prevention, Detection, Evaluation and Management of High Blood Pressure in Adults: a report of the American College of Cardiology/American Heart Association Joint Committee on Clinical Practice Guidelines. Hypertension 82, e212–e316 (2025).
Google Scholar
Beckett, N. S. et al. Treatment of hypertension in patients 80 years of age or older. N. Engl. J. Med. 358, 1887–1898 (2008).
Google Scholar
Warwick, J. et al. No evidence that frailty modifies the positive impact of antihypertensive treatment in very elderly people: an investigation of the impact of frailty upon treatment effect in the HYpertension in the Very Elderly Trial (HYVET) study, a double-blind, placebo-controlled study of antihypertensives in people with hypertension aged 80 and over. BMC Med. 13, 78 (2015).
Google Scholar
Zhang, W. et al. Trial of intensive blood-pressure control in older patients with hypertension. N. Engl. J. Med. 385, 1268–1279 (2021).
Google Scholar
Chen, T. et al. Time to clinical benefit of intensive blood pressure lowering in patients 60 years and older with hypertension: a secondary analysis of randomized clinical trials. JAMA Intern. Med. 182, 660–667 (2022).
Google Scholar
Weiss, J. et al. Benefits and harms of intensive blood pressure treatment in adults aged 60 years or older: a systematic review and meta-analysis. Ann. Intern. Med. 166, 419–429 (2017).
Google Scholar
American Diabetes Association Professional Practice Committee 13. Older adults: standards of care in diabetes — 2025. Diabetes Care 48, S266–S282 (2025).
Google Scholar
National Institute for Health and Care Excellence. Type 2 Diabetes in Adults: Management. NICE Guideline NG28 (NICE, 2022).
Nguyen, T. N. et al. The Impact of frailty on the effectiveness and safety of intensive glucose control and blood pressure-lowering therapy for people with type 2 diabetes: results from the ADVANCE trial. Diabetes Care 44, 1622–1629 (2021).
Google Scholar
Crabtree, T., Ogendo, J.-J., Vinogradova, Y., Gordon, J. & Idris, I. Intensive glycemic control and macrovascular, microvascular, hypoglycemia complications and mortality in older (age ≥60 years) or frail adults with type 2 diabetes: a systematic review and meta-analysis from randomized controlled trial and observation studies. Expert. Rev. Endocrinol. Metab. 17, 255–267 (2022).
Google Scholar
Davies, M. J. et al. Management of hyperglycemia in type 2 diabetes, 2022. A Consensus report by the American Diabetes Association (ADA) and the European Association for the Study of Diabetes (EASD). Diabetes Care 45, 2753–2786 (2022).
Google Scholar
Holman, R. R., Paul, S. K., Bethel, M. A., Matthews, D. R. & Neil, H. A. W. 10-year follow-up of intensive glucose control in type 2 diabetes. N. Engl. J. Med. 359, 1577–1589 (2008).
Google Scholar
Mach, F. et al. 2019 ESC/EAS Guidelines for the management of dyslipidaemias: lipid modification to reduce cardiovascular risk: the Task Force for the management of dyslipidaemias of the European Society of Cardiology (ESC) and European Atherosclerosis Society (EAS). Eur. Heart J. 41, 111–188 (2019).
Google Scholar
Mach, F. et al. 2025 focused update of the 2019 ESC/EAS Guidelines for the management of dyslipidaemias: developed by the Task Force for the Management of Dyslipidaemias of the European Society of Cardiology (ESC) and the European Atherosclerosis Society (EAS). Eur. Heart J. (2025).
Google Scholar
Orkaby, A. R. et al. New statin use, mortality, and first cardiovascular events in older US veterans by frailty status. J. Am. Geriatrics Soc. 72, 410–422 (2024).
Google Scholar
Mansi, I., Frei, C. R., Pugh, M. J., Makris, U. & Mortensen, E. M. Statins and musculoskeletal conditions, arthropathies, and injuries. JAMA Intern. Med. 173, 1318–1326 (2013).
Google Scholar
Hong, S. J. et al. Treat-to-target or high-intensity statin in patients with coronary artery disease: a randomized clinical trial. JAMA 329, 1078–1087 (2023).
Google Scholar
Zoungas, S. et al. Statins for extension of disability-free survival and primary prevention of cardiovascular events among older people: protocol for a randomised controlled trial in primary care (STAREE trial). BMJ Open. 13, e069915 (2023).
Google Scholar
Joseph, J. et al. Pragmatic evaluation of events and benefits of lipid lowering in older adults (PREVENTABLE): trial design and rationale. J. Am. Geriatrics Soc. 71, 1701–1713 (2023).
Google Scholar
Lewington, S. et al. Blood cholesterol and vascular mortality by age, sex, and blood pressure: a meta-analysis of individual data from 61 prospective studies with 55,000 vascular deaths. Lancet 370, 1829–1839 (2007).
Google Scholar
Van Gelder, I. C. et al. 2024 ESC guidelines for the management of atrial fibrillation developed in collaboration with the European Association for Cardio-Thoracic Surgery (EACTS): developed by the Task Force for the Management of Atrial Fibrillation of the European Society of Cardiology (ESC), with the special contribution of the European Heart Rhythm Association (EHRA) of the ESC. Endorsed by the European Stroke Organisation (ESO). Eur. Heart J. 45, 3314–3414 (2024).
Google Scholar
Mendelson, G. & Aronow, W. S. Underutilization of warfarin in older persons with chronic nonvalvular atrial fibrillation at high risk for developing stroke. J. Am. Geriatrics Soc. 46, 1423–1424 (1998).
Google Scholar
Antani, M. R. et al. Failure to prescribe warfarin to patients with nonrheumatic atrial fibrillation. J. Gen. Intern. Med. 11, 713–720 (1996).
Google Scholar
Waldo, A. L., Becker, R. C., Tapson, V. F. & Colgan, K. J. Hospitalized patients with atrial fibrillation and a high risk of stroke are not being provided with adequate anticoagulation. J. Am. Coll. Cardiol. 46, 1729–1736 (2005).
Google Scholar
Corvol, A. et al. Use of anticoagulants for atrial fibrillation in older subjects across different countries: Cyprus, France, Netherlands, Norway. Eur. Geriatric Med. 5, 60–65 (2014).
Google Scholar
Radholm, K. et al. Atrial fibrillation (AF) and co-morbidity in elderly. A population based survey of 85 years old subjects. Arch. Gerontol. Geriatr. 52, e170–e175 (2011).
Google Scholar
Monte, S. et al. Antithrombotic treatment is strongly underused despite reducing overall mortality among high-risk elderly patients hospitalized with atrial fibrillation. Eur. Heart J. 27, 2217–2223 (2006).
Google Scholar
Cohen, N. et al. Warfarin for stroke prevention still underused in atrial fibrillation: patterns of omission. Stroke 31, 1217–1222 (2000).
Google Scholar
Jackson, S. L., Peterson, G. M., Vial, J. H., Daud, R. & Ang, S. Y. Outcomes in the management of atrial fibrillation: clinical trial results can apply in practice. Intern. Med. J. 31, 329–336 (2001).
Google Scholar
Søgaard, M. et al. Net clinical benefit of oral anticoagulation among frail patients with atrial fibrillation: nationwide cohort study. Stroke 55, 413–422 (2024).
Google Scholar
Proietti, M. et al. Frailty prevalence and impact on outcomes in patients with atrial fibrillation: a systematic review and meta-analysis of 1,187,000 patients. Ageing Res. Rev. 79, 101652 (2022).
Google Scholar
Andreotti, F. et al. Antithrombotic therapy in the elderly: expert position paper of the European Society of Cardiology working group on thrombosis. Eur. heart J. 36, 3238–3249 (2015).
Google Scholar
Winijkul, A., Kaewkumdee, P., Yindeengam, A., Lip, G. Y. H. & Krittayaphong, R. Clinical outcomes of patients with atrial fibrillation who survived from bleeding event: the results from COOL-AF Thailand registry. Thromb. Haemost. 124, 991–1002 (2024).
Google Scholar
Hanon, O. et al. Expert consensus of the French Society of Geriatrics and Gerontology and the French Society of Cardiology on the management of atrial fibrillation in elderly people. Arch. Cardiovasc. Dis. 106, 303–323 (2013).
Google Scholar
Joglar, J. A. et al. 2023 ACC/AHA/ACCP/HRS guideline for the diagnosis and management of atrial fibrillation: a report of the American College of Cardiology/American Heart Association joint committee on clinical practice guidelines. Circulation 149, e1–e156 (2024).
Google Scholar
Hindricks, G. et al. 2020 ESC Guidelines for the diagnosis and management of atrial fibrillation developed in collaboration with the European Association for Cardio-Thoracic Surgery (EACTS): the Task Force for the Diagnosis and Management of Atrial Fibrillation of the European Society of Cardiology (ESC) developed with the special contribution of the European Heart Rhythm Association (EHRA) of the ESC. Eur. Heart J. 42, 373–498 (2020).
Google Scholar
Verma, L. A., Penson, P. E., Akpan, A., Lip, G. Y. H. & Lane, D. A. Managing older people with atrial fibrillation and preventing stroke: a review of anticoagulation approaches. Expert. Rev. Cardiovasc. Ther. 21, 963–983 (2023).
Google Scholar
Akashi, S. et al. Outcomes and safety of very-low-dose edoxaban in frail patients with atrial fibrillation in the ELDERCARE-AF randomized clinical trial. JAMA Netw. Open. 5, e2228500 (2022).
Google Scholar
Lip, G. Y. H. et al. Oral anticoagulants for nonvalvular atrial fibrillation in frail elderly patients: insights from the ARISTOPHANES study. J. Intern. Med. 289, 42–52 (2021).
Google Scholar
Kim, D. H. et al. Frailty and clinical outcomes of direct oral anticoagulants versus warfarin in older adults with atrial fibrillation. Ann. Intern. Med. 174, 1214–1223 (2021).
Google Scholar
Søgaard, M., Ording, A. G., Skjøth, F., Larsen, T. B. & Nielsen, P. B. Effectiveness and safety of direct oral anticoagulation vs. warfarin in frail patients with atrial fibrillation. Eur. Heart J. Cardiovasc. Pharmacother. 10, 137–146 (2024).
Google Scholar
Joosten, L. P. T. et al. Safety of switching from a vitamin K antagonist to a non-vitamin K antagonist oral anticoagulant in frail older patients with atrial fibrillation: results of the FRAIL-AF randomized controlled trial. Circulation 149, 279–289 (2024).
Google Scholar
de Jong, M. J. et al. Intra-individual variability of direct oral anticoagulant levels in frail older patients upon, during, and after acute hospitalization: the DOAC-FRAIL study. J. Am. Med. Dir. Assoc. 25, 105280 (2024).
Google Scholar
Bendayan, M. et al. Muscle mass and direct oral anticoagulant activity in older adults with atrial fibrillation. J. Am. Geriatrics Soc. 69, 1012–1018 (2021).
Google Scholar
Nissan, R. et al. Apixaban levels in octogenarian patients with non-valvular atrial fibrillation. Drugs Aging 36, 165–177 (2019).
Google Scholar
Byrne, R. A. et al. 2023 ESC guidelines for the management of acute coronary syndromes: developed by the Task Force on the Management of Acute Coronary Syndromes of the European Society of Cardiology (ESC). Eur. Heart J. 44, 3720–3826 (2023).
Google Scholar
Vrints, C. et al. 2024 ESC guidelines for the management of chronic coronary syndromes: developed by the Task Force for the Management of Chronic Coronary Syndromes of the European Society of Cardiology (ESC) endorsed by the European association for Cardio-Thoracic Surgery (EACTS). Eur. Heart J. 45, 3415–3537 (2024).
Google Scholar
Levine, G. N. et al. 2016 ACC/AHA guideline focused update on duration of dual antiplatelet therapy in patients with coronary artery disease: a report of the American College of Cardiology/American Heart Association Task Force on Clinical Practice Guidelines: an update of the 2011 ACCF/AHA/SCAI guideline for percutaneous coronary intervention, 2011 ACCF/AHA Guideline for Coronary Artery Bypass Graft Surgery, 2012 ACC/AHA/ACP/AATS/PCNA/SCAI/STS Guideline for the Diagnosis and Management of Patients With Stable Ischemic Heart Disease, 2013 ACCF/AHA Guideline for the Management of ST-Elevation Myocardial Infarction, 2014 AHA/ACC Guideline for the Management of Patients With Non–ST-Elevation Acute Coronary Syndromes, and 2014 ACC/AHA Guideline on Perioperative Cardiovascular Evaluation and Management of Patients Undergoing Noncardiac Surgery. Circulation 134, e123–e155 (2016).
Google Scholar
Kleindorfer, D. O. et al. 2021 Guideline for the prevention of stroke in patients with stroke and transient ischemic attack: a guideline from the American Heart Association/American Stroke Association. Stroke 52, e364–e467 (2021).
Google Scholar
Biondi-Zoccai, G. et al. Oral antiplatelet therapy in the elderly undergoing percutaneous coronary intervention: an umbrella review. J. Thorac. Dis. 12, 1656–1664 (2020).
Google Scholar
Ko, D. et al. Utilization of P2Y12 inhibitors in older adults with ST-elevation myocardial infarction and frailty. Am. J. Cardiol. 207, 245–252 (2023).
Google Scholar
Ko, D. et al. Frailty and clinical outcomes of ticagrelor versus clopidogrel in older adults with acute myocardial infarction. J. Am. Heart Assoc. 13, e034529 (2024).
Google Scholar
Berger, J. S. Aspirin for primary prevention — time to rethink our approach. JAMA Netw. 5, e2210144 (2022).
Google Scholar
Montgomery, S., Miedema, M. D. & Dodson, J. A. Aspirin and statin therapy for primary prevention of cardiovascular disease in older adults. Heart 108, 1090–1097 (2022).
Google Scholar
Hubbard, R. E., O’Mahony, M. S., Calver, B. L. & Woodhouse, K. W. Plasma esterases and inflammation in ageing and frailty. Eur. J. Clin. Pharmacol. 64, 895–900 (2008).
Google Scholar
Williams, F. M., Wynne, H., Woodhouse, K. W. & Rawlins, M. D. Plasma aspirin esterase: the influence of old age and frailty. Age Ageing 18, 39–42 (1989).
Google Scholar
Nguyen, T. N. et al. Effect of frailty and age on platelet aggregation and response to aspirin in older patients with atrial fibrillation: a pilot study. Cardiol. Ther. 5, 51–62 (2016).
Google Scholar
Liu, Y., Liu, S., Wang, K. & Liu, H. Association of frailty with antiplatelet response among elderly Chinese patients with coronary artery disease undergoing percutaneous coronary intervention. Clin. Appl. Thromb. Hemost. 26, 1076029620915994 (2020).
Google Scholar
Talha, K. M. et al. Frailty and heart failure: state-of-the-art review. J. Cachexia Sarcopenia Muscle 14, 1959–1972 (2023).
Google Scholar
Sharma, Y., Horwood, C., Hakendorf, P. & Thompson, C. Benefits of heart failure-specific pharmacotherapy in frail hospitalised patients: a cross-sectional study. BMJ Open. 12, e059905 (2022).
Google Scholar
Usman, M. S. et al. Sodium-glucose co-transporter 2 inhibitors and cardiovascular outcomes: a systematic review and meta-analysis. Eur. J. Prev. Cardiol. 25, 495–502 (2018).
Google Scholar
Rådholm, K. et al. Effects of sodium-glucose cotransporter-2 inhibitors on cardiovascular disease, death and safety outcomes in type 2 diabetes — a systematic review. Diabetes Res. Clin. Pract. 140, 118–128 (2018).
Google Scholar
Hamada, T. et al. Frailty interferes with the guideline-directed medical therapy in heart failure patients with reduced ejection fraction. ESC Heart Fail. 10, 223–233 (2023).
Google Scholar
Lee, Y. C. et al. Frailty and uptake of angiotensin receptor neprilysin inhibitor for heart failure with reduced ejection fraction. J. Am. Geriatr. Soc. 71, 3110–3121 (2023).
Google Scholar
Khan, M. S. et al. Frailty, guideline-directed medical therapy, and outcomes in HFrEF: from the GUIDE-IT trial. JACC Heart Fail. 10, 266–275 (2022).
Google Scholar
Kondo, T. et al. Physical frailty and use of guideline-recommended drugs in patients with heart failure and reduced ejection fraction. J. Am. Heart Assoc. 12, e026844 (2023).
Google Scholar
Butt, J. H. et al. Sacubitril/valsartan and frailty in patients with heart failure and preserved ejection fraction. J. Am. Coll. Cardiol. 80, 1130–1143 (2022).
Google Scholar
Dewan, P. et al. The prevalence and importance of frailty in heart failure with reduced ejection fraction — an analysis of PARADIGM-HF and ATMOSPHERE. Eur. J. Heart Fail. 22, 2123–2133 (2020).
Google Scholar
Neuen, B. L. et al. SGLT2 inhibitors for the prevention of kidney failure in patients with type 2 diabetes: a systematic review and meta-analysis. Lancet Diabetes Endocrinol. 7, 845–854 (2019).
Google Scholar
Arnott, C. et al. Sodium-glucose cotransporter 2 inhibition for the prevention of cardiovascular events in patients with type 2 diabetes mellitus: a systematic review and meta-analysis. J. Am. Heart Assoc. 9, e014908 (2020).
Google Scholar
Yi, T. W. et al. Kidney and cardiovascular effects of canagliflozin according to age and sex: a post hoc analysis of the CREDENCE randomized clinical trial. Am. J. Kidney Dis. 82, 84–96.e1 (2023).
Google Scholar
Butt, J. H. et al. Efficacy and safety of dapagliflozin according to frailty in heart failure with reduced ejection fraction: a post hoc analysis of the DAPA-HF trial. Ann. Intern. Med. 175, 820–830 (2022).
Google Scholar
Butt, J. H. et al. Efficacy and safety of dapagliflozin according to frailty in patients with heart failure: a prespecified analysis of the DELIVER trial. Circulation 146, 1210–1224 (2022).
Google Scholar
Coats, A. J. S. et al. Efficacy of empagliflozin in heart failure with preserved ejection fraction according to frailty status in EMPEROR-Preserved. J. Cachexia Sarcopenia Muscle 15, 412–424 (2024).
Google Scholar
Vart, P. et al. Efficacy and safety of dapagliflozin in patients with chronic kidney disease across the spectrum of frailty. J. Gerontol. A Biol. Sci. Med. Sci 79, glad181 (2024).
Google Scholar
Mayne, K. J. et al. Frailty, multimorbidity and polypharmacy: exploratory analyses of the effects of empagliflozin from the EMPA-KIDNEY trial. Clin. J. Am. Soc. Nephrol. 19, 1119–1129 (2024).
Google Scholar
Nguyen, T. N. et al. The efficacy and safety of canagliflozin by frailty status in participants of the CANVAS and CREDENCE trials. J. Am. Geriatrics Soc. 73, 1787–1796 (2025).
Google Scholar
Kim, D. H., Cheslock, M., Sison, S. M., Orkaby, A. R. & Schwartz, A. W. eFrailty: making frailty assessment accessible to clinicians and researchers. J. Am. Geriatr. Soc. 73, 318–322 (2025).
Google Scholar
Kyriakou, E., Tzefronis, D., Dagianta, G. & Triantafyllopoulos, I. K. Implementing frailty assessment into a healthcare system: a clinical opinion paper. J. Frailty Sarcopenia Falls 4, 111–115 (2019).
Google Scholar
Aliberti, M. J. R., Arteaga-Vargas, D. F. & Avelino-Silva, T. J. Frailty matters — why isn’t it guiding clinical decisions? J. Am. Geriatrics Soc. 73, 1665–1670 (2025).
Google Scholar
Ruiz, J. G. & Muscedere, J. The ethics of frailty: a need for consensus guidelines. J. Nutr. Health Aging 28, 100265 (2024).
Google Scholar
link